Introduction
Hello! My name is Abhay Sheeri, a rising sophomore at the University of Pittsburgh. I am currently pursuing a Molecular Biology major as well as a minor in Chemistry and a certificate in the Conceptual Foundations of Medicine on the premedical track. I am extremely motivated to participate in the Health Sciences Research Fellowship for the summer of 2022 and delve into the depths of my project! While this fellowship provides me with the opportunity to engage in my project, its true value is in the interdisciplinarity across the Health Sciences. The ability to connect with other undergraduate students conducting tangential research is truly a means for greater communication and exchange of ideas, something which is a vital skill in my prospective career. I was originally born in The Woodlands, Texas, but was raised in Chesterfield, New Jersey for all of my childhood. Coming from a primary suburb area, the urban life at Pitt is something I have always aspired to. The ability to engage in a multitude of activities and develop priceless connections is truly special and is what Pitt is renowned for after all. Outside of academics, I enjoy spending time outdoors and trying new ventures, like ziplining, for which I had the amazing opportunity to partake in a Service-Learning Trip of mobile clinics in Ecuador with an organization called MEDLIFE.
My Project
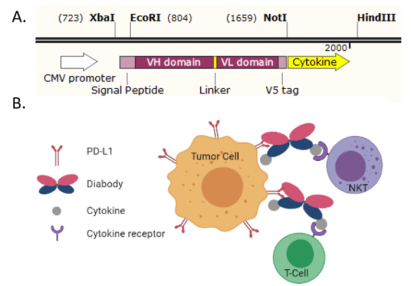
My research takes place at UPMC Hillman Cancer Center under Dr. Ravi Patel (P.I./Mentor) and Dr. Robert Edinger (Direct Supervisor). I have been in Dr. Patel’s lab for over nine months working on learning and practicing several methods required to undergo my project this summer. For the HSRF, my project focuses on immunotherapy. Immunotherapy is a form of treatment that makes use of the body’s own immune system (e.g. T-cells, cytokines) to launch an immune response against tumor cells which is in contrast to more traditional forms of treatments such as radiotherapy, surgery, and chemotherapy which are directly tumoricidal. My project fits into the preclinical phase of developing a new immunocytokine that combines two different therapies, immune checkpoint blockade and cytokine therapy into a single novel multi-functional protein structure (PDL1-IL15) to initiate cell death. I will first study the toxicity and dosing of the PDL1-IL15 diabody that our lab has developed and then perform preliminary efficacy studies in preventing metastatic spread in a preclinical mouse model of a carcinogen-induced lung cancer model, FVBW-17. After determining toxicity and a dosing regimen of our immunocytokine, we can utilize this agent to prevent distant metastatic failure after surgery or ablative radiation.
Goals
As with any project, obtaining significant quantifiable results will enable me to progress further within the scope of the project itself. More specifically, one challenge is obtaining enough of a yield of PDL1-IL15 to proceed with animal studies and successfully developing a stable cell line that expresses PDL1-IL15 which will enable us to have a consistent supply of the protein. However, I believe my project holds importance not only in its short-term results but especially in its long-term connection to evolving cancer patient treatment. Currently, with my protein of interest being assessed with mouse models in understanding tumor regression, with greater knowledge and promising preclinical results, it will enable us to transition into a clinical model, to fully understand the effects of these combination treatments on patients, such as determining safety, preliminary dosage levels, and treatment durations. The end result is to hopefully devise a new form of treatment for patients with cancer, bringing greater tumor regression and patient survival.
